Mennonite Health Journal
Articles on the intersection of faith and health
Tanzania Reflections
Winona Houser, MD
from Mennonite Health Journal, Vol. 16, No. 3 – August 2014
 I had the privilege of spending a month on rotation at Shirati KMT (Tanzanian Mennonite Church) Hospital this past winter during my final year of medical school, made possible in part through a Student Elective Term (SET) Scholarship from Mennonite Healthcare Fellowship (MHF). This was a rich experience that complemented and expanded my U.S.-based training.
I had the privilege of spending a month on rotation at Shirati KMT (Tanzanian Mennonite Church) Hospital this past winter during my final year of medical school, made possible in part through a Student Elective Term (SET) Scholarship from Mennonite Healthcare Fellowship (MHF). This was a rich experience that complemented and expanded my U.S.-based training.
On my very first morning in the hospital, I followed one of the house physicians as he completed rounds on the thirty or so patients in the female ward—an open-air ward with most of its patients admitted due to infectious disease (malaria, HIV, ectopic pregnancies secondary to pelvic inflammatory disease). Finished, he strolled to one of the cabinets in the nurses’ station, opened it, and took out a tiny kitten, which he proceeded to pet for a few moments before continuing on to the pediatric ward. For some reason, this stands out to me most vividly as the moment I acknowledged that I wasn’t in a U.S. hospital anymore: not the different case mix, or the paper charts, or the lack of patient privacy, or the language barrier, but the presence of free-range animals on hospital property.
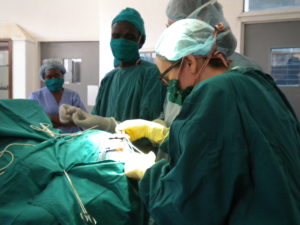 Four weeks went by quickly. The first two weeks, I worked with an American general surgeon who travels to Shirati yearly to operate. We saw a full complement of both elective and emergent cases which kept the operating theater staff busy. The last two weeks, I worked with the full-time hospital staff—all Tanzanian, with the exception of two Dutch doctors. I did rounds on post-operative patients, checked in on children with severe anemia from malaria, sat with laboring women, accompanied a team on a mobile prenatal and well-child clinic, stitched up lacerations from accidents, and assisted with a skin graft for a wound from a snake bite. I helped with amputations, D & Cs, vaccinations, and cleaning out a compound femur fracture from a motorbike accident. I watched patients die, and I watched patients recover.
Four weeks went by quickly. The first two weeks, I worked with an American general surgeon who travels to Shirati yearly to operate. We saw a full complement of both elective and emergent cases which kept the operating theater staff busy. The last two weeks, I worked with the full-time hospital staff—all Tanzanian, with the exception of two Dutch doctors. I did rounds on post-operative patients, checked in on children with severe anemia from malaria, sat with laboring women, accompanied a team on a mobile prenatal and well-child clinic, stitched up lacerations from accidents, and assisted with a skin graft for a wound from a snake bite. I helped with amputations, D & Cs, vaccinations, and cleaning out a compound femur fracture from a motorbike accident. I watched patients die, and I watched patients recover.
Throughout the whole rotation, the central question I felt humming inside me was: “Can I see myself doing this in the future?” I’m beginning my residency now, in family medicine. A desire to develop skills that would be of use in meaningful service to underserved populations fueled my decision to become a physician. I know that I’ll spend my career working with communities that have limited access to good medical care. What I don’t know yet is where that will be. My month in Shirati was an ideal time to consider whether an international setting might fit.
 I think the answer could be “Yes.” Given that my training will be in primary care, I see international work as a long-term endeavor. I thought a good bit about the unique challenges and rewards of living and working in a place like Shirati. Aside from some of the obvious differences—like the necessity of learning to navigate a different language, or managing infectious diseases unique to the place—many of the challenges are similar to those we work with in the states. There are hospital politics to reckon with. The ideal or textbook treatment may not be available (like the doxycycline I had planned to use for malaria prophylaxis—a supply shortage in the US made it prohibitively expensive for me, and I had to find an alternative). A treatment order might not be carried out as intended. There are cultural differences in the understanding and treatment of disease. Flexibility and creativity are commodities. There is joy and gratitude, there is grief and despair. There is always room for improvement.
I think the answer could be “Yes.” Given that my training will be in primary care, I see international work as a long-term endeavor. I thought a good bit about the unique challenges and rewards of living and working in a place like Shirati. Aside from some of the obvious differences—like the necessity of learning to navigate a different language, or managing infectious diseases unique to the place—many of the challenges are similar to those we work with in the states. There are hospital politics to reckon with. The ideal or textbook treatment may not be available (like the doxycycline I had planned to use for malaria prophylaxis—a supply shortage in the US made it prohibitively expensive for me, and I had to find an alternative). A treatment order might not be carried out as intended. There are cultural differences in the understanding and treatment of disease. Flexibility and creativity are commodities. There is joy and gratitude, there is grief and despair. There is always room for improvement.
Special Notes:
Students: With the beginning of the 2014-15 school year, it is not too early to begin planning for SET in 2015-16! Visit the SET web page
Any MHF member: The new Steven Roth Memorial Grant Program is accepting grant through September 15. The purpose of the Grant Program is to aid MHF members around the world as they work in educational and/or service-oriented purposes which contribute to the missional purposes of the church. Visit Grant Program page for details.
About the author
 Winona Houser, MD, is a 2014 graduate of Penn State College of Medicine. In June 2014, she moved to Asheville, North Carolina where she is completing her residency training in family medicine at MAHEC (Mountain Area Health Education Center). In her spare time away from the hospital and clinic, she enjoys exploring the nearby mountains, puttering in her small backyard garden, and reading an occasional novel.
Winona Houser, MD, is a 2014 graduate of Penn State College of Medicine. In June 2014, she moved to Asheville, North Carolina where she is completing her residency training in family medicine at MAHEC (Mountain Area Health Education Center). In her spare time away from the hospital and clinic, she enjoys exploring the nearby mountains, puttering in her small backyard garden, and reading an occasional novel.
